Multiple sclerosis is a complex condition that affects the central nervous system, leading to a wide range of challenges for those diagnosed. Early and accurate identification is crucial for managing the disease effectively and improving quality of life. This guide explores the intricate process involved in determining if someone has this condition, drawing from established medical practices to provide clear insights.
Understanding the journey toward a diagnosis begins with recognizing the signs that prompt medical attention. Many individuals experience subtle changes that gradually intensify, prompting them to seek professional help. Healthcare providers play a key role in piecing together these indicators through thorough evaluations.
The path to confirmation often involves multiple steps, ensuring that other potential causes are ruled out. This meticulous approach helps avoid misdiagnosis and tailors subsequent management strategies. Patients are encouraged to actively participate by keeping detailed records of their experiences.
Advancements in medical technology have refined the methods used, making the process more precise over time. From initial consultations to advanced imaging, each phase contributes valuable information. This comprehensive method underscores the importance of specialized care in neurology.
Recognizing the Symptoms of Multiple Sclerosis
Symptoms can vary widely among individuals, often appearing in episodes that come and go. These manifestations result from damage to the protective covering of nerves, disrupting communication within the body. Awareness of these signs is the first step in seeking timely medical intervention.
Common experiences include sensations that affect daily activities, such as mobility and sensory perception. Some people notice changes in their vision or coordination early on, while others might deal with more internal issues like fatigue. Tracking these over time can provide crucial clues for healthcare professionals.
Different forms of the condition may present unique patterns, influencing how symptoms evolve. For instance, in some cases, issues might remit partially before returning, while in others, they progress steadily. This variability highlights the need for personalized assessment.
Key Symptoms to Watch For
- Vision Problems: Blurred or double vision often stems from inflammation of the optic nerve. This can cause pain during eye movement and temporary loss of sight in one eye. Regular eye check-ups can help monitor these changes effectively.
- Numbness or Tingling: Sensations like pins and needles typically occur in the face, arms, or legs. These feelings may come on suddenly and affect one side of the body more than the other. They result from interrupted nerve signals and can vary in intensity over time.
- Fatigue: An overwhelming sense of tiredness that doesn’t improve with rest is common. This can interfere with work, social activities, and daily routines. Managing energy levels through pacing and lifestyle adjustments becomes essential for those affected.
- Muscle Weakness: Difficulty in lifting objects or walking due to reduced strength in limbs. This often affects the legs first, leading to stumbling or falls. Physical therapy can help strengthen muscles and improve overall mobility.
- Balance and Coordination Issues: Dizziness or unsteadiness when standing or walking, sometimes accompanied by tremors. These problems can make simple tasks challenging and increase the risk of injury. Assistive devices may be recommended to enhance stability.
- Bladder Dysfunction: Frequent urges to urinate or difficulty controlling the bladder. This can lead to discomfort and affect sleep patterns. Dietary changes and medications are often used to manage these symptoms effectively.
- Cognitive Changes: Trouble with memory, concentration, or problem-solving. These can impact professional performance and personal relationships. Cognitive rehabilitation strategies can assist in coping with these alterations.
- Pain and Spasms: Sharp or chronic pain, along with involuntary muscle contractions. These can occur in various body parts and disrupt sleep. Pain management techniques, including medications and relaxation exercises, provide relief for many.
These symptoms often fluctuate, making it important to note their frequency and triggers. Environmental factors like heat can exacerbate them, a phenomenon known as Uhthoff’s sign. Discussing these patterns with a doctor aids in building a complete picture.
In some instances, emotional aspects such as mood swings or depression accompany physical symptoms. Addressing mental health is integral to overall well-being. Support groups and counseling can offer valuable resources during this period.
As symptoms progress, they may impact sexual function or cause bowel irregularities. Open communication with healthcare providers ensures comprehensive care. Lifestyle modifications often play a significant role in symptom management.
The Diagnostic Process for Multiple Sclerosis
Diagnosing this condition requires a multifaceted approach, combining clinical observations with advanced testing. Neurologists specialize in this area, guiding patients through the necessary evaluations. The goal is to confirm the presence of characteristic damage while excluding similar disorders.
The process typically starts with a detailed discussion of medical history and current complaints. This helps identify patterns consistent with the disease. Following this, a series of examinations and tests are conducted to gather objective evidence.
Time is a factor, as confirmation may require observing changes over months. Patience is key, as rushing can lead to inaccuracies. Regular follow-ups allow for monitoring and adjustments as needed.
Recent revisions to diagnostic guidelines have incorporated new biomarkers, enhancing accuracy. These updates reflect ongoing research and improve the speed of identification. Staying informed about these developments benefits both patients and providers.
Initial Consultation and Medical History
The first step involves a thorough review of past health issues, family background, and symptom timeline. Doctors inquire about onset, duration, and any remitting patterns. This information helps differentiate from other neurological conditions.
Patients should prepare by listing all symptoms, even seemingly minor ones. Noting exacerbating factors, like stress or temperature changes, provides additional context. Honesty ensures the most accurate assessment possible.
Family history of autoimmune diseases may be relevant, as genetic factors can play a role. Discussing previous illnesses or exposures aids in ruling out environmental triggers. This foundational step sets the stage for further investigations.
Physical and Neurological Examination
A comprehensive physical check assesses overall health, focusing on nervous system function. Tests evaluate reflexes, muscle strength, and sensory responses. Abnormalities in these areas can indicate underlying issues.
Coordination tasks, such as finger-to-nose testing, reveal balance problems. Walking assessments detect gait irregularities. These hands-on evaluations provide immediate insights into potential nerve damage.
Vision tests check for color perception and field of view restrictions. Cognitive screening may include simple memory exercises. Results from this exam guide the selection of subsequent diagnostic tools.
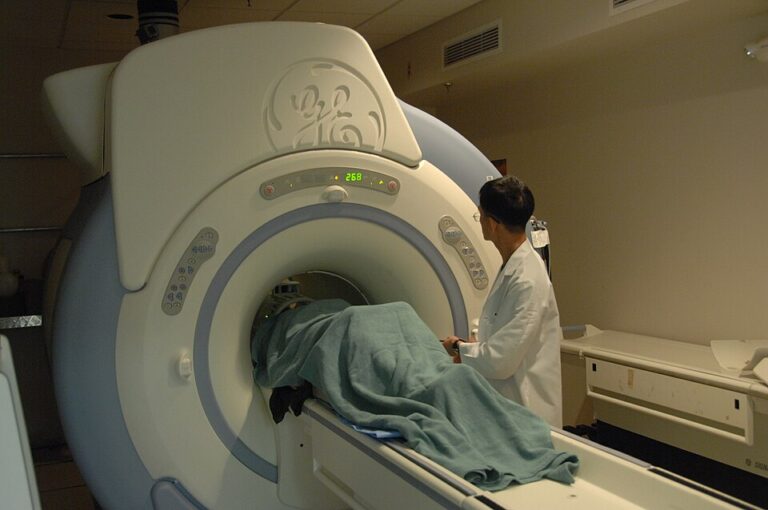
Magnetic Resonance Imaging (MRI) Scans
MRI is a cornerstone in identifying characteristic lesions in the brain and spinal cord. This non-invasive test uses magnetic fields to produce detailed images. Lesions appear as areas of scarring or inflammation.
Contrast agents may be injected to highlight active areas of disease. Scans typically last 30 to 60 minutes, requiring stillness in a enclosed machine. Claustrophobia can be managed with sedation if necessary.
Follow-up MRIs monitor progression or response to treatments. Interpreting results requires expertise, as not all findings confirm the condition. This test often provides the first visual evidence of damage.
Preparation involves removing metal objects and informing technicians of implants. The procedure is safe, with no radiation exposure. Results are usually available within days, informing next steps.
Lumbar Puncture (Spinal Tap)
This procedure involves extracting cerebrospinal fluid from the lower back for analysis. It detects elevated proteins or specific antibodies associated with the condition. The test helps differentiate from infections or other inflammatory diseases.
Performed under local anesthesia, it takes about 30 minutes. Patients lie on their side while a needle is inserted between vertebrae. Mild discomfort or headache may follow, relieved by rest and hydration.
Laboratory examination looks for oligoclonal bands, indicative of immune activity. Results can support a diagnosis when imaging is inconclusive. This test is particularly useful in progressive forms.
Evoked Potential Tests
These measure the speed of nerve signals in response to stimuli. Visual, auditory, or sensory versions assess pathway integrity. Delays suggest demyelination, a hallmark of the disease.
Electrodes are placed on the scalp or skin, with no pain involved. Tests last 20 to 40 minutes each. They provide functional data complementing structural imaging.
Visual evoked potentials involve viewing patterns on a screen. Somatosensory tests use mild electrical pulses on limbs. Abnormal results strengthen the case for diagnosis.
Blood and Other Laboratory Tests
Blood work rules out mimicking conditions like vitamin deficiencies or infections. Specific markers for alternative disorders are checked. Emerging biomarkers may soon aid direct confirmation.
Urine analysis occasionally supplements, detecting related complications. These tests are quick and performed in outpatient settings. Normal results help narrow down possibilities.
Genetic testing isn’t routine but may be considered in familial cases. Comprehensive panels ensure thorough exclusion of differentials. This step is essential for diagnostic accuracy.
Optical Coherence Tomography (OCT)
OCT scans the retina to measure nerve fiber thickness. Thinning indicates optic nerve damage common in the condition. This quick, painless test uses light waves for high-resolution images.
Performed in eye clinics, it takes minutes per eye. Results correlate with disease severity and progression. It’s increasingly used for monitoring over time.
Combining OCT with other tests enhances diagnostic confidence. It’s particularly valuable when vision symptoms predominate. Regular use can track subtle changes invisible to standard exams.
Applying Diagnostic Criteria
Guidelines like the McDonald criteria integrate clinical and test findings. They require evidence of lesions separated in time and space. Updates allow earlier identification using fluid biomarkers.
Dissemination in space means damage in multiple central nervous system areas. Dissemination in time involves lesions of different ages. Meeting these confirms the diagnosis.
For primary progressive forms, additional criteria include steady worsening over a year. These standards ensure consistency across practitioners. Periodic revisions incorporate new research.
Ruling Out Other Conditions
Differential diagnosis is critical, as many disorders mimic symptoms. Conditions like neuromyelitis optica or Lyme disease are excluded through specific tests. This prevents inappropriate treatments.
Blood tests for antibodies distinguish related autoimmune issues. Imaging patterns help differentiate strokes or tumors. Thorough evaluation minimizes errors.
In rare cases, biopsies may be needed, though uncommon. Collaboration among specialists ensures comprehensive review. This step protects patient safety and optimizes outcomes.
Types of Multiple Sclerosis and Their Diagnostic Implications
Different forms influence presentation and diagnostic approach. Relapsing-remitting is most common, with clear episodes. Diagnosis is often straightforward with supportive tests.
Progressive types may require longer observation for confirmation. Criteria adaptations allow for these variations. Understanding the type guides prognosis discussions.
Clinically isolated syndrome represents an initial event, potentially evolving. Monitoring determines if it progresses. Early intervention can alter the course in some cases.
Rare variants like tumefactive forms present unique challenges. Specialized imaging distinguishes them. Accurate typing ensures appropriate management strategies.
Pro Tips for Navigating the Diagnosis
- Keep a Symptom Journal: Document daily experiences, including triggers and severity. This aids doctors in identifying patterns. Review it before appointments for comprehensive discussions.
- Seek a Specialist Early: Consult a neurologist experienced in this area. They have access to advanced tools and knowledge. Referrals from primary care speed the process.
- Prepare for Tests: Research procedures to reduce anxiety. Follow pre-test instructions carefully. Bring a support person if needed for comfort.
- Manage Expectations: Understand diagnosis may take time. Stay informed through reputable resources. Focus on controllable aspects like health habits.
- Advocate for Yourself: Ask questions about results and next steps. Request second opinions if uncertain. Active involvement improves satisfaction with care.
- Address Emotional Health: Seek counseling for stress during waiting periods. Join support networks for shared experiences. Mental well-being supports physical health.
- Monitor Lifestyle Factors: Maintain balanced nutrition and exercise. Avoid heat if it worsens symptoms. These habits support overall resilience.
Frequently Asked Questions
Is there a single test to diagnose MS?
No definitive single test exists; diagnosis relies on a combination of history, exams, and multiple tests. This approach ensures accuracy by considering all evidence.
How long does the diagnostic process typically take?
It varies from weeks to months, depending on symptom clarity and test availability. Some cases require observation over time for confirmation.
What if my symptoms are mild?
Even subtle signs warrant evaluation, as early detection improves management. Don’t dismiss changes; report them promptly.
Can MS be misdiagnosed?
Yes, due to overlapping symptoms with other conditions. Thorough testing minimizes this risk.
Are there genetic tests for MS?
Genetic factors contribute, but no routine test diagnoses it. Research continues in this area.
What happens after diagnosis?
Treatment planning begins, focusing on symptom management and disease modification. Regular monitoring follows.
Can children be diagnosed with MS?
Yes, though rarer; pediatric cases require specialized approaches. Symptoms may differ slightly.
Does diagnosis affect life insurance?
It may impact premiums; disclose accurately when applying. Some policies accommodate pre-existing conditions.
Conclusion
Navigating the diagnosis of multiple sclerosis involves understanding symptoms, undergoing various tests, and applying established criteria. Early recognition and thorough evaluation lead to better outcomes. With advancements in medical practices, individuals can access effective management strategies to maintain quality of life. Staying informed and proactive empowers those affected to handle the challenges ahead.